Case
18 history
Dates of sampling 10. Dec.
2001 & 10. February 2003 ++
HISTORY:
Male, born 1952.
Family and previous history:
His father died only 51 years old due to myocardial
infarction. He has therefore been screened for lipid, cholesterol with
normal results.
In his twenties he had a stomach ulcer, but that
healed on antacids and he has not had any problems with that since.
He has been diagnosed with lichen planus /
lichen ruber when about 20 years old, that gave him many problems for 10-15
years, but less problems with this skin affection for the last 5-10 years. Read
Lennhoff’s interesting article from 1948, he
found spirochaetes in many skin diseases !
Since childhood he has had occasional migraine
with aura, but he can often break the attack by taking acetylsalicylic
acid with codeine.
About 4 years prior to first test he was involved
in two car-accidents and got whip-lash lesion both times, but luckily no severe
injuries, both whiplashes were treated with physiotherapy with good effect
both times, but since then he's had increasing problems with pain in
his neck, back, shoulders and tension-type headache. He has developed a saddle-neck.
Exposure to ticks:
He has planted a young vineyard and is very often working out there from spring to autumn. The roe-deer are grassing in the back yard and like fresh wine leaves very much and claws marks are all over the vineyard. The cats always have multiple ticks on them from February to November-December in mild winters.
Daughter gets multiple tick bites every year and had
two EMs in 1999 and his wife also get multiple tick bites every year and has a history
with chronic Borreliosis (EM x 3), Ehrlichiosis and Babesiosis since 1996.
So – though he's never recognized a tick bite on
himself, he's probably in very high risk for tick-exposure and getting
multi-infected right at home, and in May 1999
he developed a relatively dark erythema migrans rash about 8-
The dark EM rash disappeared within a few weeks on
this treatment, but for a long time – the scar is still visible ! – he had sort
of a dark blue / black spot on his right lower leg reminding me a bit of a eschar / tâche noire
(Rickettsial scab or ulcer) or , see picture (clip from lowres. Video) from 12.
Nov. 2000:
– and since R. helvetica was found in ticks in Bornholm and Northern Jutland, i.e. the most far apart ‘ends’ of Denmark, as well as in Sweden – so some of our local ticks on the island in the middle of Denmark – Fyn – may very well be infected with this pathogen too ? – making Rickettsia another possible co-infection to be acquired from ticks?
After treatment he remained relatively well for quite
some time, except for his usual problems that he knew before (described under
previous .. above), but during the next year he gradually began experiencing
increasing fatigue, worse headaches, waxing and vaning and wandering joint
pains, so bad that he often had to stay home from work or do his work from
home, later in the day when feeling a little better. He is an engineer by
education, but works for 10 years as a computer software consultant in
hotline function, his area is mainly production planning and logistics.
In April 2001 he had a bout of chills,
headache and developed a few petecchia
around his ankles, but these went away in few days, and he also recalls
having another similar episode, but not exactly when it was. He did not
want to contact GP at that time since it went away so fast and didn’t bother
him much. Thus I did suspect a possible relapse of borreliosis for some
time, but he was not sick enough to be motivated for testing.
On 17. Nov. 2001 had a beginning migraine
attack that was cleared with a codein + aspirin drug, before developing a
severe headache, but when he woke up the next
morning, he had again developed a petecchial rash now spreading all over his
legs, without any accompanying symptoms. Pictures were taken and GP
contacted and he was immediately referred to a practising dermatologist, who
took two consecutive skin biopsies, that showed leukocytoclastic
vasculitis - and blood samples revealed increased ALAT and
slightly increased IgA, with IgA precipitates in the vessels – AKA Schönlein-Henoch Purpura, a disease of unknown etiology
especially well known in children, that can last for a few weeks or continue
prolonged for months to years, where the vasculitis may eventually affect the
inner organs, especially the kidneys and can rarely cause kidney failure.
During the following weeks he had weekly bouts / waves of new petecchia, plus systemic symptoms; he was very fatigued, had headache and felt very restless in his legs and has a very odd sensation of 'like fluid running down his skin' just before the new bout of petecchia develop.
Since I was already running the pilot project on
chronically ill people suspect for having persistent active borreliosis, in
whom I have noticed a tendency – although never as much as in case 18 – to
develop petecchia during flares usually coming either at weekly or monthly
intervals ! – I did blood microscopy of unstained wet drop and Diff-Quik
stained peripheral blood smear and found ‘moving granulated cellular
structures’, as well as suspect ring forms in red blood cells, and also
some bigger than normal dark blue ‘granules’ included in the cytoplasm of a few
white blood cells …
Bowen-test 10. Dec. 2001 confirmed
my suspicion of him having triple TBI: RIBb positive,
babesia, HME.
So ultimo December 2001 –
April 2002 he got treatment with doxycycline, on which his headaches, joint
pain (shoulder worst) and gradually also the skin eruptions disappeared and he
got reasonably well.
Meanwhile he had been
referred to Odense University Hospital (OUH), Denmark (2-4 months waiting time
!), to the dermatology and infectious disease departments, colleagues there
chose not to take mine nor Bowen RTIs picture documented microscopy findings
serious and dismissed him after doing only one negative pair of peripheral
blood smear microscopic examination for ring forms and offering him no
treatment for the ring formed parasites ! – because they couldn’t find anything
wrong with him now !
During the summer time there
were only small eruptions of vasculitis, not serious enough to act on.
However, in November 2002
he first get a relapse of lichen rubber / planus
both skin and oral, plus the same vasculitis rash,
which increased in localisation, severity and accompanying symptoms at weekly
intervals – to becoming much worse than last years eruption – so he was re-investigated at OUH
dermatology department from december 2002.
Since the hospital colleagues had blamed his first
vasculitis eruption in 2001 on his use of acetylsalicylic acid preparation for
headache and had blamed his increased liver-enzymes on long-term intake of
‘high dose’ (i.e. children dose after weight) doxycycline, despite
his liver enzymes had actually been found elevated weeks BEFORE start of
doxycycline treatment ! – I strictly forbid him to use any drugs at all, so
they couldn’t blame the new eruption on these things this time ! – and apart
from doing a wet blood drop microscopy, I did not intervene in order to get him
properly evaluated in the hospital, also because I was in a bad relapse myself
and unable to do proper smear microscopy (takes 4-5 hours !), but I did see
many moving granulated cellular structures in his blood, which I told the
hospital colleagues and asked them to do blood smear
evaluation for parasites, which he was denied !!!??? - giving him no
logical nor any scientific arguments why not, he only got a statement in a
letter after a conference decision in the ID department:
“we can’t help you with testing because we don’t agree with US doctors on
the matter of Borrelia and Babesia” !
The most scaring symptom he had back then was some
minutes of blindness, probably caused by cerebral or retinal vasculitis / spasm
?
– luckily this has only happened once and his sight was fully restored, but he
dared not drive car for the next 2 months
…
The disease was ongoing and gradually increasing in
severity and extent so they took his case serious this time and did a lot of
tests for infections (bloodsamples, X-ray of shoulder and teeth, throat swap – which
was positive for streptococci – for which they gave him penicillin for 10
days which lead to improvement, however within 1-2 weeks after stopping
penicillin all symptoms were again increasing, now a re-culture of the throat
was negative for streptococci, AST/ASH was within normal range, and his WBC,
CRP and SR was not elevated, as would have been expected, if it was an invasive
streptococcal infection inducing his vasculitis! – against logic they still
REFUSED TO CONSIDER AND TEST FOR ANY TBI !!!!
Objective findings:
1.
A nearly
universal petecchial rash, sparing only the upper part of his
truncus and arms (T-shirt area):
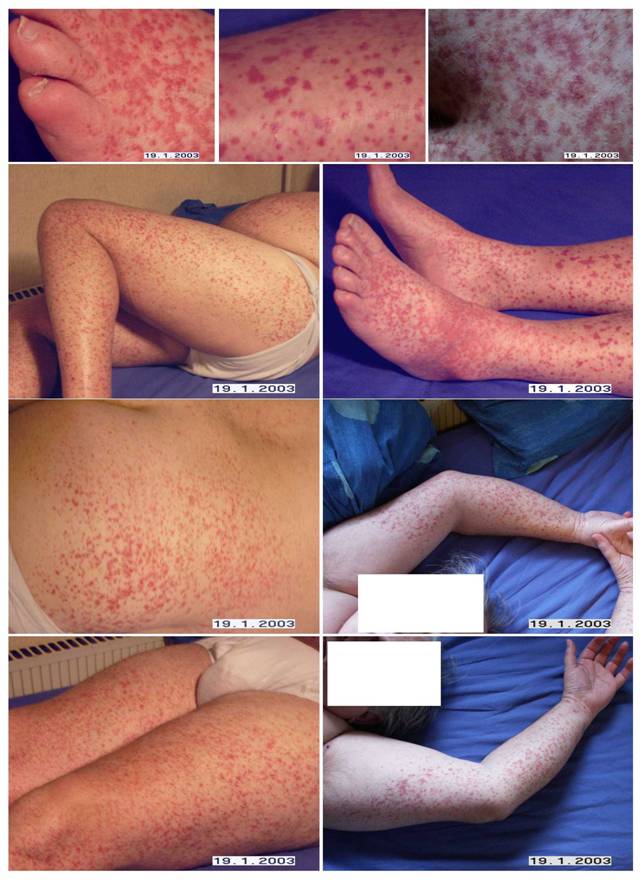
2. there was a quick (weekly) cyclical symptom attack pattern of new petecchia – very characteristic for persistent active borreliosis – while the older eruptions fade away within in a few days to a weeks time !
3.
intermittent proteinuria during the most severe vasculitis attacks
4. more skin biopsies shows lichen planus and leukocytoclastic vasculitis with IgA deposits in capillaries, plus slightly increased IgA in serum
5.
Slightly increased liver enzymes
6.
ultrasound of abdominal organs
reveal slight steatosis hepatis (he’s
overweight
7. Normal leucocytes, CRP, ESR and normal AST/ASH and no sign of viral hepatitis either
8. Normal x-ray of lungs and heart (he’s had cough and one attack of tachycardia lasting some minutes came while resting in bed),
9. Normal X-ray of shoulder and teeth ….
Since he was getting worse and worse every week, and
the hospital wouldn’t offer him any test for it, we decided to send another set
of samples to Bowen RTI on 10. February 2003, which came back
positive on Q-RIBb (low titer) and Babesia like ring forms in RBCs, but there was
no sign of Ehrlichia this time.
The ID department wouldn’t even see
him during the second and worst and of long duration attack, not even after the
second positive test for Borrelia burgdorferi ANTIGEN and Babesia came back
positive again !!!!
He was also quickly dismissed from the dermatology department and instead
referred to a rheumatologist, who followed him at rare intervals (3
months) compared to the dermatology
department (2 weeks) for about 6-8 months, while I treated him with
metronidazole and azithromycin with very good effect and gradual clearing of
all his symptoms.
The choir of doctors all sang the same tune: “well,
his disease does not belong within our specialty” – but where did such a
patient belong then, nobody could tell ?
IMO the medical specialization has gone way too far,
when the holes between the specialities and the ‘tunnel vision’ of the
specialists become so narrow that too many complex patients like case 18 fall
into the “unwanted patient category”, that NO publically payed doctor really
cares about handling !?
In this country we have a tradition, that all sick have free medical care and
of course every individual deserve the same high degree medical care and
expertise – but it seems that patients are apparently not equal human beings
any more !?
He stopped his antibiotic treatment in late July 2003
after 4 months and have had only minor bouts of petecchia since that time (last
time shortly after New Year). He is gradually feeling and functioning better –
brain wise.
He began working in April 2004 after 15-16 months sick
leave. Could that sick period perhaps have been shortened, if the public
medical system had offered him the tests and treatment that is usually
recommended in USA for Babesia and Borrelia ?
He still had a few ‘granulated cellular structures’
last time I checked a few months ago, so we reckon there is risk of relapse as well
as getting re-infection, but it’s no use worrying and forgetting to live life
on the good days J
What puzzles me, is that none of my colleagues were
willing to grab the message of a new – hitherto unsought infection, like ring
forms in RBCs – that could perhaps be the hitherto unknown cause of a ‘disease
of unknown aetiology’ like Schönlein-Henoch / “allergic” purpura !’
I would have thought that the only right thing to do, was to search for the
aetiology, i.e. to test future sick kids and adults with this ‘syndrome’
thoroughly for all TBI and other chronic infections !
One can not hope to find the aetiology of all the old ‘syndromes’ as long as most of the medical world continue closing their eyes for the possible and to me obvious !
By being negligent the medical world deprives previously well functioning people of a possibly helpful treatment and such negligence cost these patients a lot, both in suffering, lost health, lost income, lost jobs and sometimes also lost social life and family !
This is not the first time in medical
history; there are probably still numbers of people around the world with
stomach ulcers that are not being evaluated and treated curatively for their
underlying Helicobactor pylori infection, but with antacids, diet and perhaps
surgery, despite several scientific works have been published that show that
over 90% of such patient have this chronic gastrointestinal wall infection with
yet another spiral shaped bacterium !
– when do we ever learn ?